8:00 - 16:30 (gmt +7)
Novosibirsk Research Institute of Traumatology and Orthopedics n.a. Ya.L. Tsivyan
Areas of Activity
The Institute’s Spinal Pathology Clinic provides specialized medical care to patients with acute spinal trauma, including spinal cord injuries, on a 24-hour basis.
The staff of the clinic successfully performs surgical treatment of patients with posttraumatic spinal deformities, orthopedic consequences of systemic connective tissue disorders, benign spinal and osteal tumors, and secondary vertebral destruction. In addition, the clinic provides surgical treatment to patients with peripheral skeletal pathology, posttraumatic limb bone deformities; remote consequences of spinal injuries.
Such state-of-the-art surgical techniques as advanced tumor reduction, decompressive, and stabilizing operations, including minimally invasive ones, are widely practiced in the Clinic.
The staff successfully applies advanced techniques for surgical treatment of spinal disorders and injuries using state-of-the-art metal hardware and surgical instrumentation from leading foreign and domestic manufacturers, as well as proprietary instrumentation.
The Clinic’s main scientific focus is to study spinal and spinal cord injuries and their consequences, pathological states of the vertebral column against the background of systemic disorders, such as ankylosing spondylitis and rheumatoid arthritis. The researchers aim to develop new techniques for surgical correction of deformities and spinal instability, as well as sagittal balance restoration.
Advanced technologies, state-of-the-art equipment, and the high professional standards of the personnel make it possible to effectively provide specialized medical help to patients with spinal injuries and disorders, including those with concurrent pathologies.
Pediatric and Adolescent Vertebrology Clinic specializes in treatment of spinal deformities of various origins. Their key areas of activity include providing diagnostic services and surgical treatment to children and adolescents with severe spinal deformities, including those complicated by neurological symptoms, using the most advanced corrective spinal surgery instrumentation.
In 1996, the Clinic was the first one in Russia to use the Cotrel-Dubousset instrumentation, which significantly enhanced its treatment capabilities.
The personnel has accumulated vast experience in surgical treatment of severe Scheuermann’s kyphosis. Availability of a posterior and, if necessary, of an anterior approach to the spine makes it possible to radically change the shape of the spine and improve a patient’s quality of life.
The staff of the clinic also provides medical care to patients with spinal deformities caused by neurofibromatosis, the Marfan syndrome, the Ehlers-Danlos syndrome, and other syndromal lesions. In 2009, our doctors started treating children with a rare but severe cervical spine pathology using the Vertex instrumentation. They also deal with paralytic (neuromuscular) spinal deformities. Spinal deformities are treated in patients of any age, even preschoolers, if necessary.
The surgeons also perform all types of spinal osteotomy (SPO, PSO, VCR), if it is necessary due to the severity of a case. If spinal deformities are complicated by neurological symptoms or neglected cases proprietary surgical interventions (spinal cord transposition) are performed to repair the curvature and remove spinal cord compression.
Proprietary techniques are also used to treat patients with caudal regression syndrome.
The Clinic’s key areas of scientific research include further improvement of techniques and technologies for surgical treatment of severe progressive spinal deformities of various origins, investigation of progression peculiarities and incidence of scoliosis in children in various regions, 3D simulation of spinal deformities to improve the quality of surgical treatment and its outcomes.
Pediatric Orthopedics Clinic provides a full spectrum of surgical interventions in children and adolescents with congenital and acquired musculoskeletal pathology, posttraumatic defects and deformities, postoperative relapses and complications.
In recent years, the use of biodegradable implants and minimally invasive techniques of bone growth control in children and adolescents have become key trends. In most cases, these methods make it possible to repair limb bone deformities or length discrepancies without major postoperative mobility restrictions.
The clinic has accumulated vast experience in surgical treatment of pediatric patients with infantile cerebral paralysis, congenital chest deformities, dysplasia, and hip instability.
Surgical treatment of equino-planovalgus foot deformity in children and adolescents using both classical and proprietary techniques is another rapidly developing area of the Clinic’s research.
Our doctors perform successful surgeries of orthopedic lower limb pathology (abnormal knee joint development, congenital curvature and lower leg nonunions, axial deformities in hip and knee joints, congenital lower limb shortening, and foot deformities); congenital upper limb deformities, and limb bone deformities as a result of trauma and diseases.
Patients with congenital generalized musculoskeletal deformities in need of reconstructive plastic surgery, including with external fixation, form a separate group of complex cases requiring a personalized approach.
All the patients who have undergone surgery are closely followed up by our traumatologists and orthopedists. The clinic provides personal consultations by e-mail to patients from other cities.
Surgical interventions are performed using advanced endoscopic equipment, state-of-the-art metal hardware and tissue implants, and with a personalized approach to each patient.
Neurovertebrology Clinic provides routine surgical care to patients with degenerative spinal disorders. The doctors perform both standard surgical interventions and complex decompressive-stabilizing and corrective surgery (in case of scoliosis, sagittal balance disorder, and spondyloptosis). Minimally invasive surgical techniques are widely used to minimize surgical trauma and reduce the duration of hospital stay and postoperative rehabilitation.
Our surgeons were the first ones in Russia to perform laparoscopic lumbar interbody fusion using porous titanium nickelide implants. They used a minimally invasive technique with transpedicular and interbody fixation combined with bilateral decompression by unilateral approach. Both single-stage and multi-stage surgical interventions (TLIF, LLIF, ALIF, minimally invasive vertebrotomy) are extensively used to treat patients with spinal deformities Microsurgical decompressive interventions are performed in patients in pain caused by herniated discs; decompressive-stabilizing interventions are performed in patients with spondylolisthesis and segmental instability, and spinal cord neurostimulation – in patients with neuropathic pain.
Surgical interventions are performed in compliance with the international standards and using state-of-the-art implants and hardware from leading foreign and domestic manufacturers.
In 2012, the clinic received the status of reference clinic of AOSpine in Russia, which makes it a key element of the European network of regional AOSpine centers.
The Clinic’s key areas of scientific research include improvement of methods and techniques of surgical treatment of degenerative spinal lesions, including those developed in cooperation with domestic and foreign partner institutions, and standardization of surgical treatment degenerative-dystrophic diseases and spinal deformities.
The Institute’s Neurosurgery Clinic was established in 1950 by Prof. Ksenia I. Kharitonova to become one of the first facilities of such kind behind the Urals. For more than 30 years its doctors have been studying the problems of neurooncology and developing reconstructive techniques to treat skull defects using individualized 3D – printed titanium implants. The facility employs modern microsurgical equipment such as a surgical ND laser (Dornier MedTech) as well as modern diagnostic equipment such as MR and helix CT tomographs and expert-class electrophysiological and US gages.
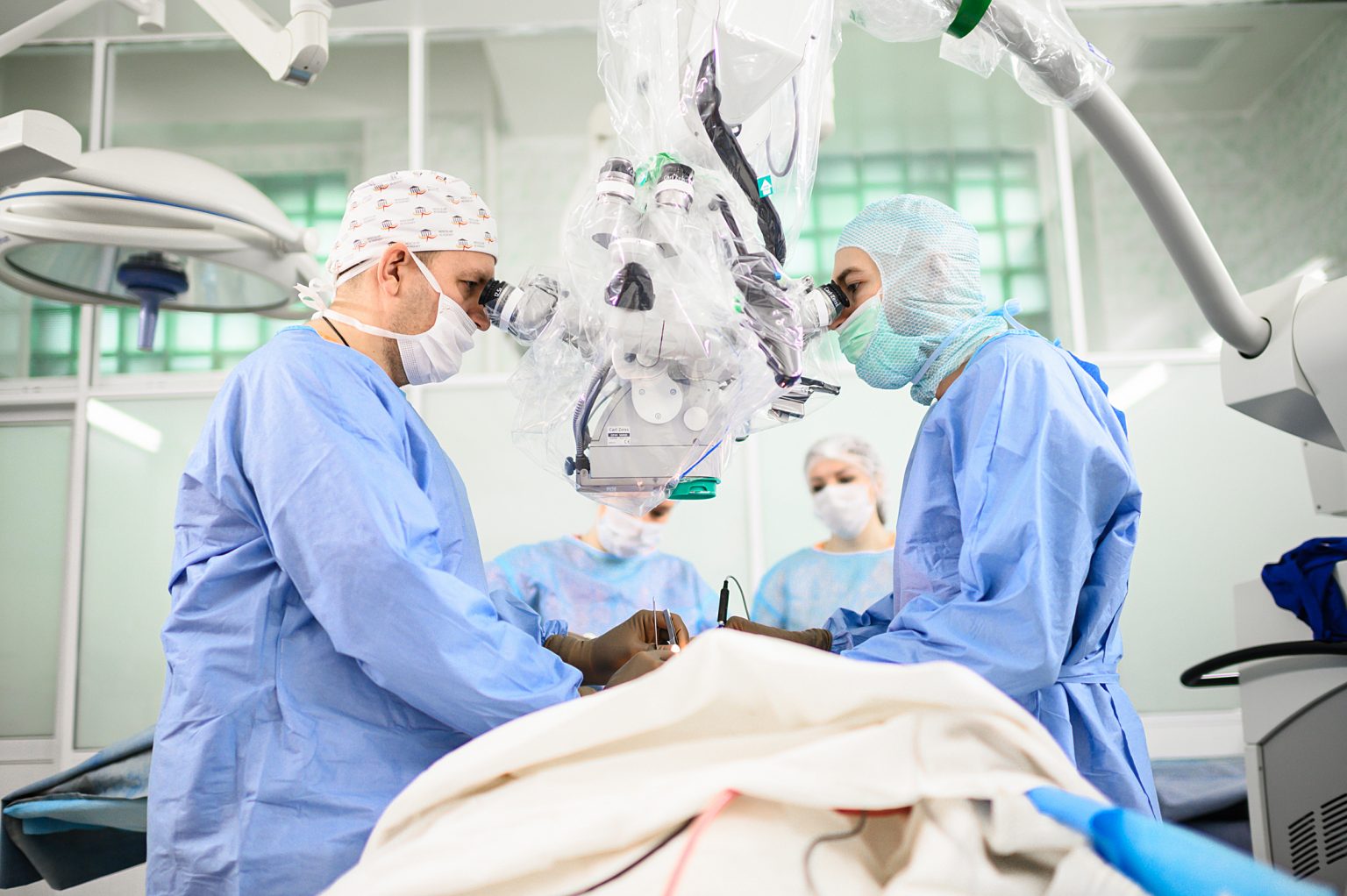
The doctors of the clinic operate patients with complex spinal and cerebral tumors of different sizes and localizations including those of the brainstem. Surgical removals of CNS tumors are carried out under electrophysiological control of brain and spinal cord functions.
The Clinic’s personnel is actively involved in research to develop new surgical techniques as infrared laser treatment of CNS meningiomas; molecular genetic testing of brain gliomas, and new methods of immunotherapy for complex treatment of malignant brain gliomas. These studies are performed in collaboration with the research institutes of the Siberian Branch of the Russian Academy of Sciences. The list of our collaborators includes Research Institute of Fundamental and Clinical Immunology; Research Institute of Cytology and Genetics; Research Institute of Molecular and Cellular Biology; N.N. Vorozhtsov Research Institute of Organic Chemistry; M.A. Lavrentiev Research Institute of Hydrodynamics; Novosibirsk State University and Novosibirsk State Medical University.
The constant development and application of state-of-the-art medical technologies and modern high-tech microsurgical equipment allow our doctors to perform the most complex microsurgical interventions.
Joint replacement is one the most perspective and fast-developing specialisms of the Institute. The doctors of our Endoprosthetics and Endoscopic Joint Surgery Clinic have gained enormous experience in treatment of all possible joint pathologies. Joint replacement here is performed in accord with international standards and employs modern prosthetic implants and the state-of-the-art equipment produced by leading Russian and foreign manufacturers.
The Clinic has been actively introducing new methods of computer-assisted surgery to build 3D models of individualized implants and developing hip revision surgery.
The doctors of the Clinic devise proprietary methods and techniques to treat a tibia medial defect and restore a kneecap while primary knee replacement.
The Clinic has gained significant success in treatment of foot pathologies; ankle-joint and first MTP joint replacements; joint-spearing and mini-invasive procedures on the knee and shoulder joints. Our doctors were the first in Russia to use ceramic prostheses to replace wrist and articulation joints.
The clinic successfully applies both primary and revision surgery techniques for shoulder joint treatment with anatomical and reversible implants; elbow joint replacement; correction of severe deformations of articulation joints due to systemic diseases; simultaneous surgery of the forearm, tendons and articulation joints.
Our traumatologists and orthopedists work together with vertebrologists to achieve an optimum result in treating patients with concomitant backbone and joint pathologies.
The Institute’s Anesthesiology and Resuscitation Service is a true frontliner when it comes to introduction and application of the most advanced techniques to provide anesthesia and intensive care. Their utmost goal is to deliver a service of the highest quality, so our patients feel safe and secure.
The Service’s scientific activities are aimed at perfecting anesthetic care for patients undergoing complex high-tech surgery of the spine and joints; improving anesthetic/intensive care strategy and tactics for spinal/interspinal injuries; correcting intestinal and nutritional insufficiency in orthopedic and elderly patients with account for their comorbidities; reducing hospital stay after large-joint replacement.
In 2012 the Service was subdivided into independent departments: of Anaesthesiology and Resuscitation and of Resuscitation and Intensive Care. Both departments employ modern expert-class equipment for general anesthesia, post-op monitoring, vital function control, constant medicinal treatment and so on.
Using state-of-the-art anesthetic equipment and techniques as well as the professionalism of our intensivists and implementation of the latest scientific developments have made it possible to significantly increase the effectiveness of the intensive care the Service provides to all our patients including infants; the elderly; those in critical conditions and significantly reduce the duration of postanesthetic resuscitation.


